Why learning to say no is part of self-advocacy in healthcare
Saying no at the right time can be the correct decision down the line
Written by |

When was the first time you heard the words “advocate” and “advocacy”?
According to Dictionary.com, to advocate means “to speak or write in favor of; support or urge by argument; recommend publicly.” And the Cambridge Dictionary says advocacy is the “public support for an idea, plan, or way of doing something.”
Are those the definitions you learned? In what context did you use these words?
Before I was diagnosed with Sjögren’s syndrome, I understood advocacy only as a civic term. For me, it didn’t extend beyond calls for justice or humanitarianism in public policy and economics. But man oh man, when Sjögren’s ushered lupus and thalassemia into my life, advocacy took on a much broader meaning.
Instead of pushing, planning, urging, or supporting something that impacted people broadly, I was jolted by these chronic conditions into a reality of pushing, planning, urging, and supporting treatments that not only affected me directly and immediately, but also that hopefully would one day lead to a cure.
Early on after my diagnoses, I had no idea I’d have to advocate for my health at every level of care, both locally and nationally.
How it began
The need to advocate for myself became apparent when I was enduring monthly trips to the emergency room and long hospitalizations because of pleurisy, chronic pain that caused myositis, and uncontrollable vomiting. For years, I had found only marginal medicinal options, low-dose painkillers, and ambivalence from doctors. This prompted an ongoing process of speaking up in order to be treated with respect and to receive proper care.
Each doctor appointment was an opportunity to be vocal about my health. Each test result gave me a chance to better understand and, if needed, a reason to challenge what it meant. Each symptom that doctors ignored forced me to speak my mind about the implications. It was a continuous process, and, as with civic advocacy, I soon learned that I had to be intentional and prepared.
I discovered in local and national support groups how important it is to ensure that notes from doctor appointments and interactions with hospital staff are accurate. I learned to trust but verify everything.
Did I say that? Did they say that? Were my symptoms and needs logged? Were they fully addressed? Were my unanswered questions documented? Were all the test results in? Did we determine the next steps and new treatments? Were any medication adjustments noted?
With questions like these, I learned a powerful advocacy strategy: saying no as a solid medical decision. It’s one thing to say, “You have the power to say no,” but it’s another to explain that saying no at the right time is a valid decision.
I’ll admit, I didn’t know when to say no until an older woman assured me that I could trust myself. At the time, I needed something to celebrate, and this validation excited me. It was only a matter of time — a few doctor appointments later, in fact — when I decided to say no. Twice.
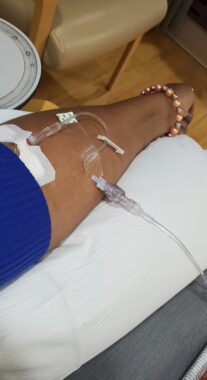
After she declined a port to help with blood tests and infusions, Candace Semien’s veins grew stronger and allowed her to receive care. (Courtesy of Candace Semien)
The first time was when chemotherapy was suggested as the next treatment option. I hadn’t been getting any relief and I’d had a near-death lupus crisis. Sill, I declined. “No. No chemotherapy,” I said confidently.
The second time I advocated for myself by saying no was after several failed attempts at drawing blood from my fragile veins. Emergency room nurses and phlebotomists tried to convince me to have a port inserted beneath my skin, just below my collarbone. “No, thank you,” I replied. Instead, I thought we could be patient and find good veins without a port.
In both situations, I was convinced that I could and would get better without either of these two things.
Understandably, these decisions created some internal conflict. I sat for a while with an unpleasant tension. I was aware that medicines could help me to heal, and saying no to a potentially innovative treatments might seem inconsistent. However, in the process I was learning to be an advocate — an advocate for me; a lupus advocate.
After I said no, my doctors and nurse practitioners offered guidance and other options to incrementally control the severity of my flares and strengthen my veins.
Then, to honor my “no,” I pushed publicly for different treatment plans and learned what researchers were working on for both lupus and Sjögren’s syndrome.
Today, I am confidently waiting for the results of new infusions I’ve had and celebrating my port-less chest!
Won’t you celebrate with me?
Note: Lupus News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Lupus News Today or its parent company, Bionews, and are intended to spark discussion about issues pertaining to lupus.


Leave a comment
Fill in the required fields to post. Your email address will not be published.