10 Frequently Asked Lupus Questions
Written by |

Because lupus is such a complex disease, it affects people differently. Because symptoms may vary from person to person, the treatments have to be personalized. But what more should you know about lupus? Here’s a list of ten of the most frequently asked questions about this chronic, autoimmune disease (source: Lupus.org website):
1. What is lupus?
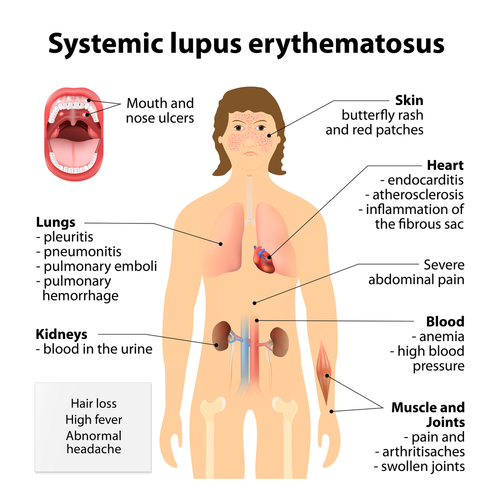
Lupus is an autoimmune inflammatory disease that affects multiple organ systems. Each patient is uniquely affected by lupus. Some of the most common symptoms of lupus include rash, joint and muscle pain, kidney disorder, and neurological disorder. Lupus is also a disease of flares (the symptoms worsen and you feel ill) and remissions (the symptoms improve and you feel better).
If you want to learn more about lupus, check this out.
2. What are the most commonly known symptoms of lupus?
Lupus affects people in different ways and symptoms vary. Some symptoms act up during periods called flares when patients may experience fatigue, headaches, sensitivity to light, joint pain, facial rashes, and a range of other symptoms — depending on the specific organs effected by lupus.
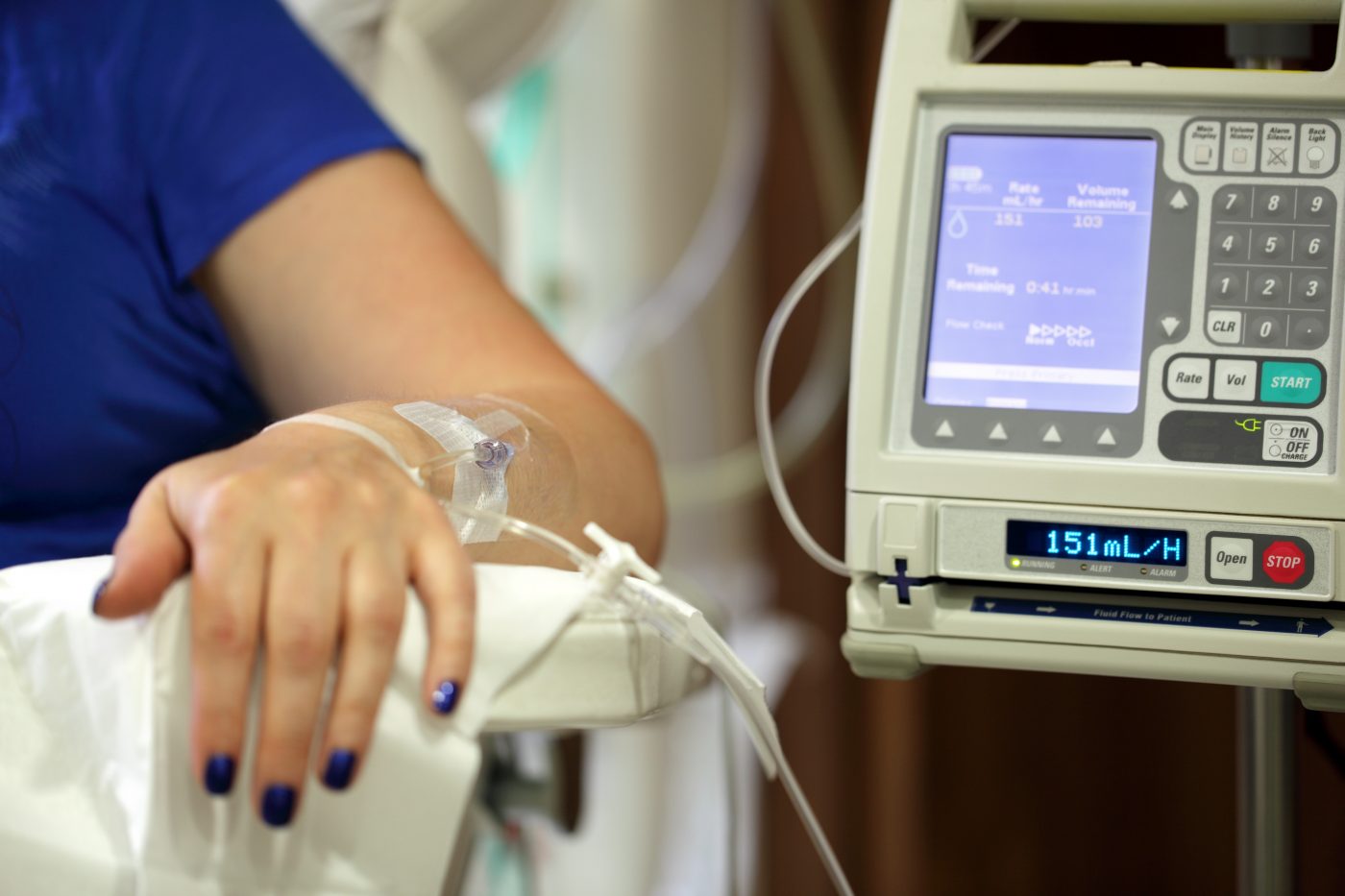
3. Is chemotherapy a treatment option for people with lupus?
Chemotherapy can be a choice of treatment depending on the patient. In certain cases people with lupus can be treated with cyclophosphamide, a chemotherapy commonly used to treat cancer.
Find out more about living with lupus and having chemotherapy as a treatment.
4. How is lupus diagnosed?
Because disease symptoms vary widely from patient to patient and symptoms can overlap with those of other diseases, lupus is difficult to diagnose.
The American College of Rheumatology defined eleven different symptoms lupus patients may experience. If an individual experiences at least four of the eleven symptoms, a physician may diagnosis lupus. Doctors use several laboratory tests, physical examinations, and patient histories to make a more accurate diagnoses.
Find out more about 13 common symptoms of lupus.
5. What are the treatment options for lupus?
There are many categories of drugs physicians use to treat lupus. However, the U.S. Food and Drug Administration has approved only a few specifically for lupus. They include:
- Corticosteroids, including prednisone, prednisolone, methylprednisolone, and hydrocortisone
- Antimalarials, such as hydroxychloroquine (Plaquenil) and chloroquine
- The monoclonal antibody belimumab (Benlysta)
- Acthar (repository corticotropin injection), which contains a naturally ocurring hormone called ACTH (adrenocorticotropic hormone)
- Aspirin
Here’s a list of 5 lupus treatment options you should know about.
6. Lupus can also affect the skin. How does this happen?
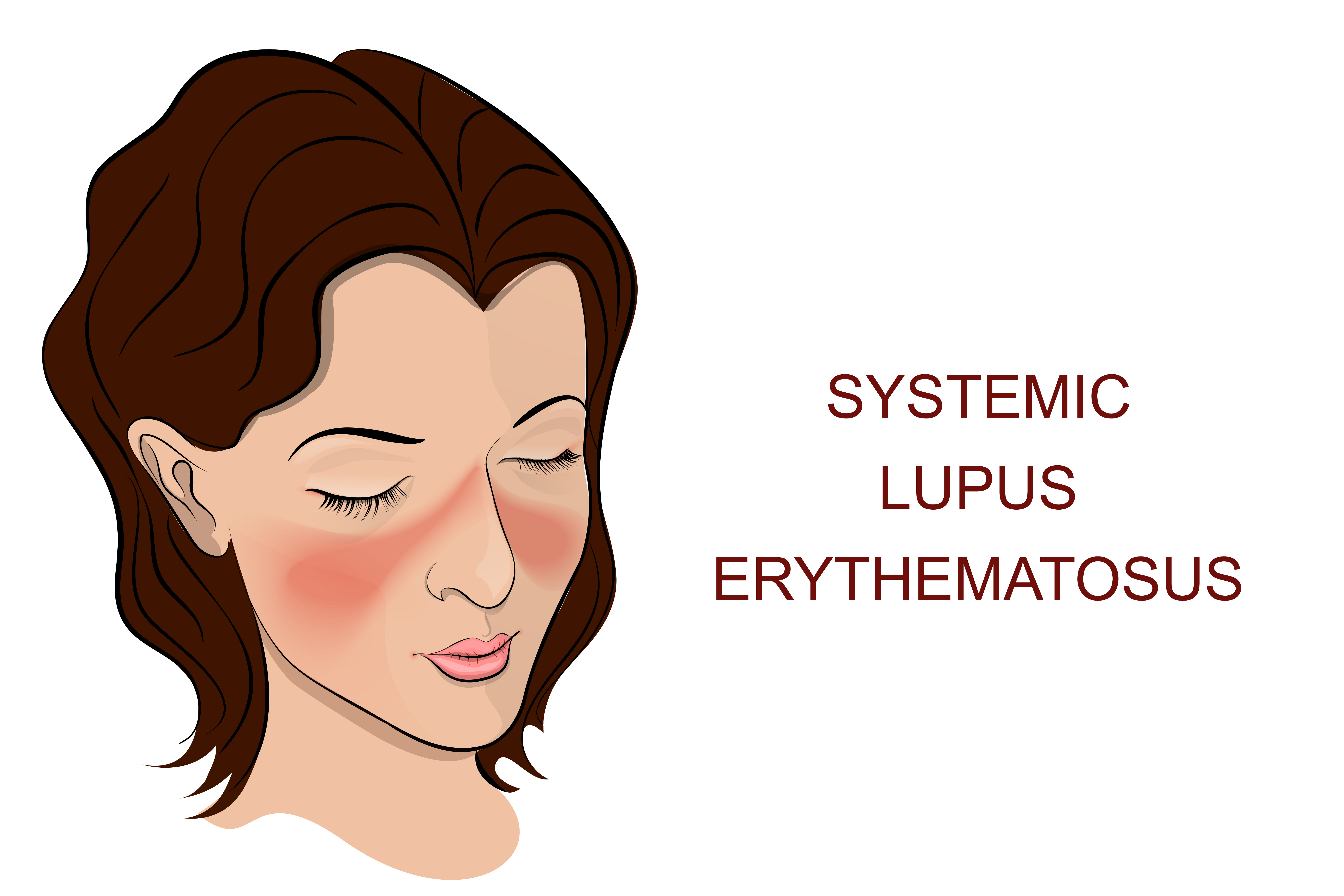
Approximately two-thirds of people with lupus have cutaneous lupus erythematosus which is lupus of the skin. Skin disease in lupus can cause rashes or sores (lesions), most of which will appear on sun-exposed areas such as the face, ears, neck, arms, and legs.
Learn more about 13 common symptoms of lupus.
7. How many types of lupus skin disease exist?
Lupus skin disease can occur in one of three forms:
1. Chronic cutaneous (discoid) lupus: Appears as disk-shaped, round lesions. The sores usually appear on the scalp and face but sometimes they will occur on other parts of the body as well.
2. Subacute cutaneous lupus: Lesions may appear as areas of red scaly skin with distinct edges or as red, ring-shaped lesions. The lesions occur most commonly on the sun-exposed areas of the arms, shoulders, neck, and body. The lesions usually do not itch or scar, but they can become discolored.
3. Acute cutaneous lupus: Lesions occur when your systemic lupus is active. The most typical form of acute cutaneous lupus is a malar rash–flattened areas of red skin on the face that resemble a sunburn. When the rash appears on both cheeks and across the bridge of the nose in the shape of a butterfly, it is known as the “butterfly rash.”
Find out more about 13 common symptoms of lupus.
8. Is there are specific diet or nutrition plan I should be following, for my lupus?
There is no special diet for lupus despite numerous claims on the internet and in various publications. You should eat a generally nutritious, well-balanced, and varied diet that contains plenty of fresh fruits and vegetables, whole grains, and moderate amounts of meat, poultry, and fish.
Check out some diet tips and changes you could do to help you manage your lupus.
9. What are common triggers for a lupus flare?
It is common for patients with lupus to feel fatigue, especially if they live high-energy lifestyles. Fatigue is one of many symptoms of a flare, making it difficult for some busy and high-energy patients to know if their exhaustion is related to lupus. Patients may experience fevers, rashes (such as facial “butterfly” rashes), increased fatigue, mouth sores, and leg pains.
Have you ever thought wondered how your immune system responds to your lupus flares?
10. Why is exercise so important in managing lupus, and what exercises could I do with lupus?
Exercise is an important way to take care of yourself, even for the extremely healthy who do not suffer from any health condition. But because exercise offers so many benefits, it is particularly helpful for people with lupus.
From a physical standpoint, exercise can strengthen parts of your body that may be affected by lupus — the heart, lungs, bones and joints. Exercise reduces inflammation by regulating some of the chemicals involved in the inflammation process, and it can reduce fatigue.
Learn more about yoga for lupus and how exercise can help patients.
Lupus News Today is strictly a news and information website about the disease. It does not provide medical advice, diagnosis or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or another qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website.